Columbia University
Irving Medical Center
Neurological Institute
710 West 168th Street, 3rd floor
(212) 305-1818
Featured Research
5th ANNUAL TAUB RETREAT
October 2014

From left to right: Badri Vardarajan, Karen Duff, Ulrich Hengst
Karen Duff's presentation explored the mechanism by which tauopathy could propagate between brain cells leading to the progressive worsening of tau pathology in AD. Using sophisticated cell culture models, the Duff lab has demonstrated that tau can be released and taken up by neurons, and experiments using conditioned media showed, for the first time, that tau can be taken up by recipient cells from the media that was used to bathe tau expressing donor cells. This indicates that tau could transfer from donor to recipient cell populations via the extracellular space either in vesicles such as exosomes, or as free tau. Of note, tau release in to the media was enhanced by neuronal activity using an optogenetic approach. Duff's lab has further demonstrated that when optogenetic stimulation was applied in vivo, tau spread between regions suggesting that in vivo stimulation also led to altered tau release. This observation may be significant in determining whether Aβ/amyloid induced hyperactivity that has been observed in APP mouse models and human AD could initiate or worsen tau propagation, and whether there may be any risk associated with human stimulation therapies such as Deep Brain Stimulation (DBS) or Transcranial Magnetic Stimulation (TMS) that are currently in clinical trials for AD. Duff also presented work from her lab that suggests a therapeutic approach based on enhancing clearance of abnormal tau forms. Duff's lab has shown that one way by which tau can accumulate in cells is due to dysfunction of proteasome mediated clearance mechanisms. From an extensive study using mouse and cell models, they demonstrated that a possible therapeutic pathway aimed at enhancing proteasome activity (PKA activation) may be effective against early stage tauopathy. They are now testing whether proteasome activation therapeutics can prevent the spread of tau pathology in vitro and in vivo. As propagation of pathology has now been implicated as a major pathogenic mechanism in other neurodegenerative diseases, these data may have relevance for proteinopathies other than AD, such as Parkinson's disease (PD), Amyotrophic Lateral Sclerosis (ALS), Huntington's disease (HD), and frontotemporal dementia (FTD).
Ulrich Hengst addressed the spread of AD through the brain, as determined by connectivity rather than proximity, and the importance of investigating how neurodegenerative signals in the periphery of neurons change intra-neuritic signaling pathways and how these signals are communicated to the neuronal cell bodies. The Hengst lab discovered a novel signaling mechanism for the long-range, retrograde spread of neurodegeneration in response to soluble oligomeric β-amyloid 1-42 (Aβ). Axonally sensed Aβ triggers intra-axonal elongation initiation factor 2α (eIF2α) phosphorylation and ATF4 synthesis. ATF4, a transcription factor, is retrogradely transported to the neuronal soma where it changes gene expression, leading eventually to cell death. Their studies identify a central role for ATF4 in AD and suggest that targeting this signaling pathway might be a promising approach to delay the progression of AD. Indeed, interference with intra-axonal ATF4 synthesis or its retrograde transport abolishes neurodegeneration both in vitro and in vivo.
Badri Vardarajan focused on applications of next generation sequencing in AD, describing two near complete projects and a few ongoing analyses in the lab. The first project, "Targeted Sequencing in SORL1 Gene," is a follow-up of an initial Taub study that implicated this gene in late onset AD (LOAD) through genome wide association studies (GWAS). This new study led to the discovery of 3 bona fide mutations in the SORL1 gene through deep sequencing in Caribbean Hispanic and Caucasian subjects from Toronto. In cell culture studies, these mutations produced more Aβ 40 and Aβ 42 compared to the wild type and all three bound to APP less efficiently than the wild type protein. The second project, "Targeted Sequencing in GWAS Identified LOAD Genes," was conducted in 8 genes identified by GWAS in three distinct cohorts. Here, Vardarajan and co-investigators observed 3.7 fold enrichment of rare coding mutations but did not see any such enrichment in the synonymous mutations in AD cases versus controls. According to Vardarajan, this suggests that the background mutation rate is the same in cases and controls, but there is a much higher rate of mutation in rare coding mutations in cases. ABCA7, which is implicated in cholesterol metabolism, was the most interesting gene, in which 10% of the cases carried at least one coding ABCA7 mutation compared to 1% controls.
William Kreisl addressed the fact that, while AD has been associated with inflammatory responses in the brain, the relationship between inflammation and AD pathology is not well understood. Kreisl demonstrated that PET imaging can quantify inflammation using 11C-PBR28, which binds to the 18 kDa translocator protein (TSPO). TSPO is over-expressed by activated microglia and reactive astrocytes. His studies have shown that 11C-PBR28 binding is greater in AD patients than in older controls and the amount of binding correlates with clinical severity and the amount of atrophy seen on MRI. 11C-PBR28 PET may therefore have potential for objectively monitoring disease progression and tracking response to novel therapeutics designed to reduce inflammation.
 William Kreisl
|
 Yunglin Gazes
|
Yunglin Gazes discussed how white matter integrity is highly correlated with cognition. She hypothesizes that unique patterns of changes in white matter integrity are age-related declines in the different cognitive abilities affected by aging: episodic memory, reasoning and perceptual speed. She showed that FA of the left Anterior Thalamic Radiation, which connects the thalamus to frontal regions, mediated the effect of age on Perceptual Speed ability. However, due to the high collinearity between white matter integrity and age, Gazes posited that advanced statistical techniques will have to be explored to tease apart the independent contributions of the two factors on cognition.
New Taub faculty member Hwamee Oh presented on Amyloid PET, Cognition, and Imaging in Aging. Even in cognitively normal older adults, beta-amyloid deposition is associated with poorer cognition in episodic memory and executive functions, greater gray matter atrophy, and increased brain activity during task performance. Oh suggests that, in combination with other neuroimaging methods, amyloid PET has the potential to increase our understanding of the neurobiology of AD. She demonstrated that the presence of amyloid in cognitively intact elders is associated with reduced efficiency of neural circuits underlying episodic and working memory. Oh stated that studying presymptomatic older adults using amyloid PET is particularly important to identify individuals at higher risk of developing AD and to develop effective intervention programs and tools for early diagnosis.
Regarding lessons learned from other neurodegenerative disorders, Brian McCabe discussed his work in Spinal Muscular Atrophy (SMA). Using a Drosophila (fruit fly) model of the disease, McCabe and co-investigators found that reduced SMN function within subsets of sensory and central neurons lead to the dysfunction of other neurons, including motor neurons, through their interconnected dependency as part of circuit assemblies. McCabe and his collaborators have subsequently validated that this novel circuit dysfunction disease mechanism also occurs in rodent models and potentially human SMA patients, and they have identified an ameliorative drug using a Drosophila model that is currently used in human clinical trials. He speculates that pathological circuit dysfunction, or 'circuitopathy', may contribute to the development and progression of other motor neuron diseases.
 Brian McCabe
|
 David Sulzer
|
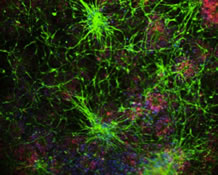
Similarly, David Sulzer's work in Parkinson's disease (PD) showed that neurons that die in affected brain regions of patients with PD remarkably act as antigen presenting cells. He also showed how the acquired immune system recognizes these antigens in patients, and suggested that this mechanism could underlie the loss of neurons over the course of PD, and other neurodegenerative disorders.
Laura Beth McIntire reported identification of a new modulator for the beta-site amyloid precursor protein (APP)-cleaving enzyme 1 (BACE1) cleavage of APP resulting from a chemical genetics screen. Pharmacological and genetic data suggest that a novel cellular target for BACE1 modulation is the plasma membrane monoamine transporter (PMAT), an atypical monoamine transporter. Further studies are on-going to understand the cellular mechanism responsible for regulation of APP cleavage by PMAT and to validate the role for PMAT in AD.
Estela Area-Gomez presented her development of a novel line of research to explain some of the early events in the pathogenesis of AD, based on observation of significant upregulation of the communication between the endoplasmic reticulum (ER) and mitochondria in cellular models of AD, via ER-mitochondrial membranes, or MAM. She hypothesizes that in AD, aberrant MAM contacts may be responsible for altered lipid metabolism and increased processing of APP through the amyloidogenic pathway.
Ray Razlighi proposed the development of a region-based spatial normalization (RBSN) technique that will increase the accuracy of data localization in brain imaging. RBSN aligns each neuroanatomical region of the human brain separately and independently. In contrast, the prevailing spatial normalization method tries to align all regions of the brain at once. RBSN will, therefore, provide more accurate localization and ensure that group analysis test the same brain area in each study participant. Better between-participant registration also provides additional statistical power to detect effects in regions that may not have reached the significance level using prevailing methods (i.e. reduce type II error). It may also rule out previously noted areas of activation that were detected for artifactual reasons (i.e., reduce type I error).