Columbia University
Irving Medical Center
Neurological Institute
710 West 168th Street, 3rd floor
(212) 305-1818
About Us
Taub Faculty
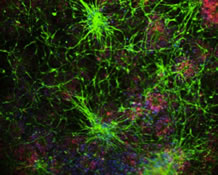
Our lab is interested in CNS glial cell development, function, and pathology. We study how astrocytes react to the presence of pathological changes and how pathological changes in astrocytes affect the other cells of the CNS.
In collaboration with Osama Al Dalahmah in Pathology and Vilas Menon in Neurology, we are using single nucleus RNASeq, a recent and powerful technique that allows us to explore gene expression of single cells of patients with neurological diseases. We have begun with Huntington disease, an inherited disorder characterized clinically by abnormal, involuntary movements and genetically by an expansion of CAG repeats in the huntingtin gene. We use fresh frozen brain specimens taken from the NY Brain Bank here at the Columbia Medical Center. In comparision to brain tissues of patients without neurological disease, we have found many significant alterations in neurons, glia, and microglia. The studies have also revealed substantial heterogeneity in transcription within individual cell types in both normal and diseased brain tissues. We are also studying transcriptional differences in the brains of individuals with Parkinson’s disease and comparing those to gene expressions in other neurological disorders.
In collaboration with Guomei Tang and David Sulzer of Neurology, Guy McKhann, Alexander Sosunov, and Xiaoping Wu of Neurosurgery, and Peter Sims of Systems Biology, we are studying the cellular and molecular changes in astrocytes and neurons that take place during the evolution of epilepsy and in the evolution of autistic-like behavior. Our collaborative group uses mouse models of Tuberous Sclerosis (TS), a disease characterized by seizures and commonly by autism-spectrum disorders, in which cells have constitutively activated mTOR. The mouse model replicates the formation of greatly enlarged neurons that are characteristic of TS and of focal cortical dysplasias. We find that these neurons are highly active and likely represent the cellular substrate of seizures. We also have performed RNASeq and ribosomal profiling and footprinting, which show us that many genes are transcriptionally regulated and also allow us to discover translationally-regulated gene expression.
As part of our studies on the neuropathology in autopsies of individuals who have died of SARS-CoV-2 infections, we discovered the deposition of amyloid protein, similar to that one sees in the brains of Alzheimer's patients. However, these individuals had no clinical or pathological signs of Alzheimer’s disease. Furthermore, we found similar deposits in the brains of people who had suffered severe hypoxia toward the ends of their lives, including children with heart anomalies.Thus, we think that these amyloid deposits are likely caused by hypoxia. We are studying what protein fragments are present in these deposits and what effects the deposits may have on brain structures in their vicinities.